Provinces Continue to Combat the Drug Crisis
Available in Audio Format:
Early in 2024, ARPA posted a 4-part article series on Canada’s drug crisis. Part 1 focuses on the nature of the drug crisis in Canada, examining its complexity and the various public policy responses to it. Part 2 considers what being created in God’s image means for a public policy response to the drug crisis. Part 3 discusses the moral responsibility of drug users, comparing drug use as a health issue and as a criminal issue. Finally, part 4 looks at what an appropriate penalty ought to be for drug use, keeping in mind problems with both the “harm reduction” and incarceration approaches and supporting a stronger treatment and recovery model.
While the principles outlined in that series remain relevant, the policy landscape has changed over the last couple of years, as has the nature of the drug crisis itself.
The Nature of the Drug Crisis
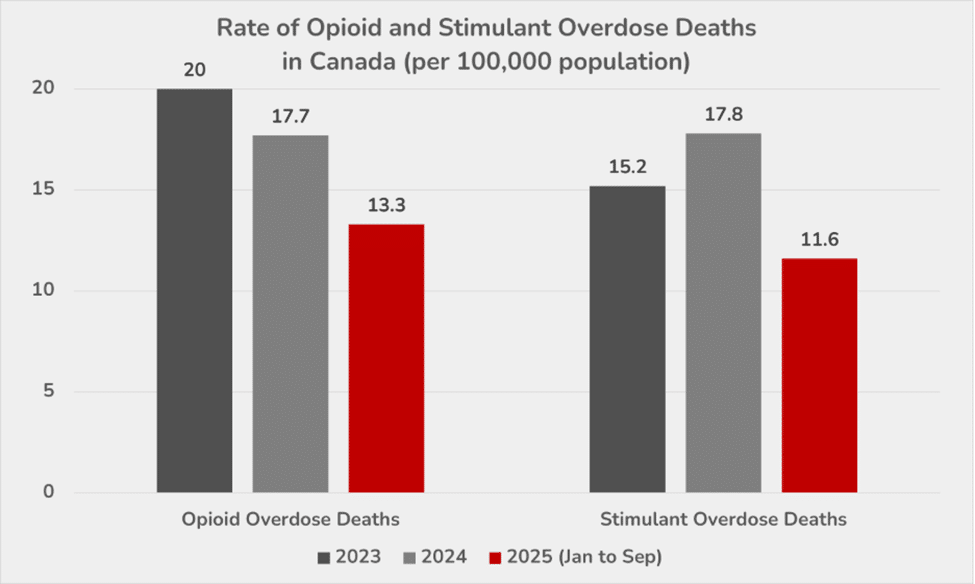
After years of increasing drug-related deaths, Canada saw a 17% decline in 2024 compared to 2023. Drug overdose deaths continued to decline in 2025. Between October 2024 and September 2025, there were 5,724 apparent opioid toxicity deaths, averaging 16 deaths per day. While this number is still alarmingly high, it is 26% lower than the previous 12 months. Similarly, in that same timeframe, there were 3,383 stimulant toxicity deaths, averaging 9 deaths per day, which was 36% lower than the previous 12 months.
Likewise, drug-related hospitalizations, emergency department visits, and EMS responses to suspected overdoses all decreased in 2025. British Columbia, Alberta, and Ontario continue to have the most drug-related deaths, though Ontario’s numbers are lower per capita than Saskatchewan and Manitoba. British Columbia, Alberta, and Yukon have the highest rates of death per capita.
It’s difficult to say why drug deaths have decreased in recent years. Health Canada identifies likely, possible, and unlikely factors.
Three likely factors include changes in the drug supply (less toxic drug combinations), better access to medication that reverses overdoses, and fewer people at risk of fatal overdose in communities. One possible factor is that people use drugs in less risky ways. Three unlikely factors include programs that test for drug contaminants, supervised consumption sites and overdose prevention sites, and medication treatment for opioid dependence.
Notably, while Health Canada says supervised consumption sites and overdose prevention sites provide important benefits and need to be combined with other approaches to reduce deaths, they also note that the limited number of sites cannot account for the reduction in deaths across the country.
The debate about the value of safe injection sites continues. When a number of injection sites in Toronto were closed in 2025, overdoses did not increase, though advocates of such sites warned that they would. Monthly fatal overdoses in that region have decreased every month since the sites closed.
A recent study out of Alberta also found that closing two sites there did not increase deaths in the region, and in fact, may have increased demand for treatment. However, the authors note that the evidence is inconclusive.
Provincial Responses to the Drug Crisis
Canadian provinces are moving towards more of a treatment-focused approach to drug addiction and away from “safe supply” and supervised injection sites. Most notable are policy developments in British Columbia, Alberta, Saskatchewan, and Ontario.
British Columbia
Early in 2023, British Columbia officially began its drug decriminalization pilot program after receiving an exemption from the federal prohibition on hard drugs. That exemption meant that, although possessing or using hard drugs is federally prohibited by the Controlled Drugs and Substances Act, the province could temporarily permit possession of small amounts of illegal drugs.
In 2024, BC’s government revised its approach slightly, permitting illegal drug possession in private spaces but not in most public spaces. Through that change, they also gave police tools to respond to public drug use, so police could seize drugs and arrest people for public drug use, if necessary.
That federal exemption from criminalizing drugs expired in January of this year, and the BC government decided not to renew it. Regarding that decision, Health Minister Josie Osborne said, “Despite the hard work and good intentions behind the pilot, it has not delivered the results we hoped for. For that reason, we will not be asking the federal government to renew the exemption.” This is a significant change. BC had been the Canadian jurisdiction most dedicated to decriminalization.
Alberta
Alberta, on the other hand, has continued its recovery-focused approach to the drug crisis with a few significant developments.
In 2025, Alberta passed the Compassionate Intervention Act to impose involuntary treatment on people who are a risk to themselves or others due to their drug use. The law establishes a Compassionate Intervention Commission composed of lawyers, physicians, and members of the public. The Commission will review applications, conduct hearings, and make orders regarding care. Family members, medical professionals, and police can refer people to the Commission for assessment. People brought to compassionate intervention centres will immediately receive treatment to stabilize and assess them. Within 72 hours of admittance, a panel of three members will hear the case and consider whether a care plan should be ordered. While the law has been passed, it has yet to be fully implemented.
The government also continues to shut down supervised consumption sites, recently announcing the closure of sites in Calgary and Lethbridge. Once those sites are closed, only three will remain in the province. Meanwhile, the Alberta government has invested in two new compassionate intervention centres in Calgary and Edmonton, with construction set to begin this year.
Saskatchewan
At the end of 2025, the Saskatchewan government introduced two bills to combat illegal drugs in the province. Both bills have yet to pass, but are expected to. The first, Bill 47, The Response to Illicit Drugs Act, seeks to increase penalties for drug traffickers, improve community safety, and give the government and individuals tools to recover costs associated with harm caused by illegal drugs. It would allow the province and individuals to pursue civil action against drug companies for drug-related harms. Saskatchewan is also working to add 500 new addiction treatment spaces.
Like Alberta, Saskatchewan has also introduced a Compassionate Intervention Act,which would create a mechanism for involuntary addiction treatment. Currently, anyone participating in treatment in the province must choose to do so. Minister of Mental Health and Addictions Lori Carr stated, “Individuals struggling with addiction need our support on their path to recovery … They need a safe space, support and compassionate intervention. We are focused on meaningful long-term recovery for Saskatchewan residents.”
The bill, if passed, would allow family members or others to request court-ordered treatment for a loved one. Law enforcement and medical professionals could also refer people to assessment centres if they believe the person is putting their own life or the lives of others at risk.
The bill would establish a Compassionate Intervention Board consisting of at least one lawyer or judge, an addiction specialist, and a community representative. One member of the board must be of Indigenous ancestry. People in need of intervention would be brought to an Assessment Centre where the panel can determine whether the person meets the threshold for involuntary treatment.
Ontario
Late in 2024, the Ontario government passed legislation requiring municipalities to obtain provincial approval before seeking federal exemptions for injection sites. The legislation also prohibited drug injection sites from operating within 200 metres of schools or daycares.
In June 2025, the province passed legislation prohibiting public consumption of illegal drugs and giving law enforcement more tools to stop people from consuming drugs publicly, including in public parks and tents in public places.
Beginning in 2025, the government began investing in 28 Homelessness and Addiction Recovery Treatment (HART) Hubs across the province. The goal of these Hubs is to connect people to treatment and support so they can break the cycle of addiction. These Hubs would also add nearly 900 supportive housing units in the province.
In 2026, the province announced that it would end provincial funding for seven drug injection sites in communities supported by a HART Hub. This includes sites in Toronto, Ottawa, Niagara, Peterborough, and London.
Conclusion
While each of these provincial approaches differs, they show a movement towards recovery-focused care for drug addiction rather than providing free drugs. The drug crisis continues to be a difficult issue to combat through public policy, but we can be grateful that governments are modifying their approach in light of evidence that “safe supply” is not safe or effective. The strong emphasis on treatment and recovery, including involuntary treatment, is relatively new in Canada and primarily a focus of specific provinces. As a result, the decrease in drug-related deaths cannot be credited to these approaches. However, we can hope and pray that these changes will help to further reduce drug deaths.